What Does Comorbid Mean
by Patient Expert
Comorbid, in medicine, refers to a disease or condition that occurs at the same time as another illness. Dictionary definitions differ:
-
Some say comorbidity refers to two or more illnesses that occur simultaneously
-
Some say it refers to one or more illnesses that occur at the same time as a primary condition.
-
Some say it refers to two or more conditions that are present at the same time and independently of each other.
In bipolar disorder, the most common comorbid conditions are anxiety disorders such as:
and others. Experts say just over 50% of people with bipolar disorder also have at least one anxiety disorder during their lives.
Studies have found that anywhere from 65% to as much as 95% of patients with bipolar have had one or more comorbid conditions in their lifetimes. Besides anxiety disorders, other psychiatric illnesses include:
-
Substance abuse disorder
-
And to be smokers
While there are many psychiatric drugs that can contribute to obesity and diabetes, these conditions have also been found to be higher than normally present in patients not taking medications.
The presence of comorbid conditions can complicate and worsen bipolar symptoms – and, in some cases, the opposite is true. This means, for one thing, that your doctor needs to be aware of all your medical and psychiatric conditions, as having more than one illness at the same time can make a lot of difference in what medications he or she prescribes.
Clinical Predictors Of High Medical Comorbidity Burden
Next, we report results of the logistic regression for predicting a high burden of general medical comorbidity. Estimates of the parameters given here are for variables that remained in the model after a stepwise selection procedure. For this regression analysis, the sample was limited to 174 of the 225 patients who had no missing information available on all of the candidate variables. Age at study entry , BMI , and a diagnosis of substance dependence were significant predictors of high medical comorbidity burden. A diagnosis of substance abuse, number of psychiatric hospitalizations, bipolar subtype, anxiety disorder comorbidity, and a history of sexual abuse were considered as candidate variables but were not significant in this sample after inclusion of the other variables.
Diagnosing Comorbid Bipolar Disorder And Substance Use Disorder
Because bipolar disorder and substance use disorder share symptoms, such as impulsivity, Isabelle Bauer, PhD, from the University of Texas Health Science Center at Houston, and colleagues thought that by measuring patients degree of impulsiveness, they could better predict treatment response.3 Patients with bipolar disorder with and without lifetime substance use disorder were given the Structured Clinical Interview for the Diagnostic and Statistical Manual of Mental Disorders Axis I , the Barratt Impulsivity Scale, and portions of the Cambridge Neuropsychological Test Automated Battery .3 To the researchers surprise, bipolar disorder chronicity or substance use disorder did not predict impulsivity.3
In bipolar disorder, high impulsivity tendencies are associated with poor clinical outcomes such as poor treatment adherence, relapse, rehospitalization, and reduced chances of going back to a normal life even after remission, explained Dr Bauer. It is unclear whether impulsivity is a symptom of bipolar disorder, or rather, the result of brain damage associated with repeated mood episodes and/or substance use.
Don’t Miss: How To Come Out Of A Bipolar Episode
What Is Panic Disorder The Symptoms And Causes And How To Get Treatment
Although one of the symptoms of BPD is anxiety, between 75 and 90 percent of people with BPD also meet criteria for at least one type of anxiety disorder, such as social anxiety disorder and panic disorder.
The difference between BPD and anxiety or panic disorders is the latter cause symptoms more frequently and for a greater period of time, for at least six months. Their anxiety is more pervasive and chronic than the anxiety that is related to BPD, Cullen says.
When To See A Doctor

Diagnosis typically involves these components:
- A physical exam
- A psychiatric evaluation
There is no single bipolar disorder test, but blood tests and neuroimaging may be used to rule out other conditions. Bipolar symptoms can resemble those of other disorders, which can make it challenging to properly diagnose the condition.
In children and teens, symptoms of bipolar disorder may be especially hard to distinguish from normal mood changes and behaviors. Children and teens in a manic episode may be irritable and short-tempered, have trouble sleeping and staying focused, and engage in risky behaviors. Those experiencing a depressive episode may complain of stomachaches and headaches, experience changes in eating habits, have little energy and interest in activities they usually enjoy, have thoughts about death and suicide.
Also Check: Are People With Schizophrenia Dangerous
Treatment Considerations For Comorbid Bd And Ptsd
Patients with comorbid BD and PTSD have a higher risk of psychosis upon hospitalization , personality disorder diagnosis , and suicide attempts .6,37 Poorer quality of life, accelerated illness progression, and high rates of functional impairment also characterize patients with this comorbidity, with a higher symptom burden compared to either illness alone.6,38,39
Non-adherence to treatment in BD increases the risk of rapid cycling, suicide attempts, current anxiety, and alcohol use disorder.40 Non-adherence at 3 month follow-up is predictive of less improvement in bipolar symptoms than non-adherence at 12 month follow-up.40 Patients with non-adherence to treatment for comorbid BD and PTSD may have childhood or other trauma that created a negative or distrustful impression of physicians, health care providers, and medication treatment.41 Traumatic outcomes resulting from dangerous behaviors that occur during a manic episode may trigger the reemergence of PTSD symptoms. Posttraumatic stress disorder nightmares could impact the sleep-wake cycle, leading to decreased sleep and a greater risk for a manic episode.41
Relationship Between Medical Comorbidity And Sud Status
Table 2 presents a summary of patient demographic, clinical, and medical comorbidity measures stratified by SUD status. Patients with co-occurring recent SUDs were more likely to be male , diagnosed with bipolar I disorder , have a history of psychosis , have experienced a manic/hypomanic/mixed episode over the 12 months prior to study entry , and to lack health care coverage . There was no significant difference in the mean CIRS total score, number of organ systems affected by medical illness, or overall number of baseline medical illnesses between the cohorts with and without co-occurring SUDs.
You May Like: How To Deal With Schizophrenia In A Relationship
Comorbid Bipolar Disorder And Substance Abuse: What To Know
Comorbidity, the presence of two or more disorders at once, is common in people with mental health struggles. There is a particularly strong link between mood disorders and drug or alcohol abuse. Bipolar disorder, a mood disorder characterized by strong highs and lows of emotion, has one of the highest rates of comorbidity with addiction. If you or a loved one is struggling with co-occurring bipolar disorder and substance abuse, you are not alone. By understanding how to recognize the signs of mental health struggles, as well as substance abuse, you can take the first steps to seek treatment.
Bmi And Response Or Remission Status
Concerning the relationship between body weight and depression, BMI was found to be a significant predictor of nonresponse and nonremission to combined treatment with lithium and valproate. For every 1-unit increase in BMI, the likelihood of responding decreased by 7.5% and the likelihood of remitting decreased by 7.3% . Obesity, but not overweight, was a significant negative predictor of remission as measured by the MADRS total score . The likelihood of attaining remission was 64.8% less likely for an obese individual compared to those in all other weight categories .
The effect of SUD status on the likelihood of achieving response differed significantly according to baseline BMI. Patients with an SUD and BMI < 23 had a greater probability of response than subjects without an SUD. However, subjects with an SUD and BMI 23 had a lower probability of response than subjects without an SUD .
Don’t Miss: How To Ground Yourself During A Panic Attack
Medical Comorbidity In Bipolar Disorder: Implications For Functional Outcomes And Health Service Utilization
The estimated lifetime prevalence of mood disorders in the general population is approximately 10 to 15 percent . From a population-health perspective, mood disorders are currently the leading cause of disability and premature death among young adults .
A mounting scientific database documents the increased prevalence of medical comorbidity among persons with a mood disorder . For example, subclinical hypothyroidism is associated with recurrent depression, longer disease duration, more frequent affective episodes, repetitive nonlethal suicidal behaviors, and a higher body mass index .
This post hoc analysis aimed to ascertain the prevalence and prognostic implications of predetermined comorbid general medical disorders amongst persons who screen positive for a manic episode. The burden of medical comorbidity on employment, functional role, psychiatric care, and medication use was examined within this subpopulation of individuals.
Signs And Symptoms Of Bipolar Disorder
There are different types of bipolar disorder, differing in symptoms and severity. A hallmark of every type is discrete mood episodes that are interspersed with periods of normal, level mood and function. Your doctor will diagnose your condition on the basis of the length, frequency, and pattern of episodes of your mania and depression.
When a person doesnt meet the criteria for any of the other types of bipolar disorder but still experiences periods of a significant, abnormal elevation in mood, they may be diagnosed with “other specified and unspecified bipolar and related disorders.”
You may feel easily distracted, as though your thoughts are racing, and be excessively talkative. You may also need less sleep. And along with an inflated sense of self-confidence, you might engage in pleasurable but reckless, risky behaviors with negative consequences.
Manic episodes involve a distinct and observable change in mood and functioning, and are severe enough to result in problems in your daily activities or to require hospitalization to prevent harm to yourself or others. A manic episode may also trigger a break from reality , including hallucinations or delusions.
Don’t Miss: How To Stop Aids Phobia
Rates Of Medical Illnesses Across The Bipolar Unipolar And Control Groups
The lifetime rates of self-reported medical illnesses in the bipolar, unipolar and control groups are shown in Table 1. Significant differences between groups were found in the lifetime prevalence of all medical illnesses with the exception of type 1 diabetes.
To examine differences in the rate of each medical illness between the three groups, accounting for gender and age at interview, binary logistic regression was carried out for all medical illnesses showing a significant between-group difference in the univariate analyses. Diagnostic group was entered as the outcome variable and presence/absence of the medical disorder, gender and age at interview were entered as cofactors. Odds ratios, 95% confidence intervals and P-values for each logistic regression analysis are shown in Table 2. Following correction for multiple testing, using the Bonferroni method, statistically significant differences in the rates of ten medical illnesses remained between the three groups .
Table 1 Lifetime rates of self-reported medical illnesses in bipolar, unipolar and control groups
| Medical illness |
|---|
a. Data only available for a subset of the bipolar disorder group .
How Can You Receive A Diagnosis With Both Conditions

Most people who have a dual diagnosis of bipolar disorder and BPD receive one diagnosis before the other. Thats because the symptoms of one disorder can overlap and sometimes mask the other.
Bipolar disorder is often diagnosed first because symptoms can change. This makes it more difficult to detect BPD symptoms. With time and treatment for one disorder, the other may become clearer.
Pay a visit to your doctor and explain your symptoms if you think youre showing signs of bipolar disorder and BPD. Theyll likely conduct an assessment to determine the nature and extent of your symptoms.
Your doctor will use the newest edition of the Diagnostic and Statistical Manual to help them make a diagnosis. Theyll review each of your symptoms with you to see if they align with the other disorder.
Your doctor will also consider your mental health history. Often, this can provide insight that can help distinguish one disorder from the other. For example, both bipolar disorder and BPD tend to run in families. This means if you have a close relative with one or both of the disorders, youre more likely to have them.
The treatments of bipolar disorder and BPD are different because each disorder causes different symptoms.
Bipolar disorder requires several types of treatment, including:
BPD is primarily treated with talk therapy the same type of therapy that can help treat bipolar disorder. But your doctor may also suggest:
You May Like: What Percent Of The Population Has Depression
Resources For Family And Friends
The mission of the Depression and Bipolar Support Alliance is to educate, support, and help people living with a mood disorder and the people closest to them. This community-like website offers in-person and online support groups, as well as videos, programs, and a Wellness Toolbox for family and friends.
Comorbid Bipolar Disorder And Obsessive
- Edward S. Andrea Michael E. Friedman Fagiolini ThaseHandbook of Mental Health in the Workplace2002
- Personality Disorders: Toward the DSM-V2007
- Susan M. Swearer and more…Encyclopedia of School Psychology
- The SAGE Encyclopedia of Intellectual and DevelopmentalDisorders2018
- Paul C. McCabe and more…Psychiatric Disorders: Current Topics and Interventions for Educators2010
- The SAGE Encyclopedia of Abnormal and Clinical Psychology2017
- Rachel L. Loewy and more…Handbook of Clinical Interviewing with Children2007
- Introduction to Abnormal Child and Adolescent Psychology2008
- Psychotic Disorders in Children and Adolescents2001
You May Like: What Are Treatments For Eating Disorders
Do You Have A Codependent Personality
Narcissistic personality disorder People have an inflated sense of self, a deep need for excessive attention and admiration, troubled relationships, and a lack of empathy for others.
Avoidant personality disorder People have feelings of inadequacy and are constantly afraid that others will criticize them, so they avoid situations and interactions with others.
Dependent personality disorder People have a strong need to be taken care of and have a fear of losing support from others.
Obsessive-compulsive personality disorder People are preoccupied with control and perfectionism and often neglect relationships in favor of orderliness.
The Relationship Between Bipolar Disorder And Sex Drive
During manic episodes, people with bipolar disorder may engage in certain impulsive behaviors. For some people, this kind of behavior can involve a preoccupation with sex and a heightened sex drive, leading to unprotected sex or risky sexual situations with potentially damaging consequences, both physical and emotional. Hypersexuality, or an increased interest in sex, is known to be a symptom of bipolar disorder, though the research on the subject is limited.
Learn More About Bipolar Disorder and Sex Drive
Read Also: Does Spencer Reid Have Schizophrenia
Bipolar Disorder: Sorting Out Comorbidities
Because patients with bipolar disorder often have underlying comorbidities, a thorough diagnosis is imperative.
It is important to identify comorbid disorders that add to the symptoms of bipolar disorder, so that these symptoms can be targeted appropriately. Some prescribers tend to target symptoms with medications while leaving the underlying disorder unrecognized and/or untreated.
The evaluation may require several meetings to reach the initial diagnostic impression, and it can take 90 minutes to evaluate a complex new patient, including reviewing the previous record and writing the assessment.Experienced clinicians may convince themselves that they can do an adequate assessment in less time and choose the correct medications for the correct diagnoses. However, a competent and comprehensive psychiatric evaluation requires time. Brief evaluations, followed by quick prescribing, are often experienced by patients as rushed and unsatisfying. Confidence in and respect for our profession can be undermined by these practices.
It is important to make this diagnosis, using the DSM-5 criteria, and consider which symptoms could be attributed to ADHD and which occur mostly or to a greater extent during discreet manic episodes.
Read the original article here.
Medical Comorbidity In Relation To Symptom Severity And Treatment Response
Of the combined sample of 225 patients with and without a recent SUD, 50.7% were male, 69.8% had bipolar I disorder, and 75.1% had a lifetime comorbid anxiety disorder. Their mean age was 36.8 years. The mean number of baseline medical comorbidities per patient was 2.5 . The mean CIRS total score was 4.3 , and the mean number of organ systems affected was 3.1 . The rates of bimodal response to the combination of lithium and valproate by CIRS total score among subjects with and without a comorbid SUD are reported in Table 1. A total of 47% of patients had a moderate burden of medical comorbidity , whereas 8% of patients had a severe burden .
Recommended Reading: How To Help Someone With Bipolar Depression
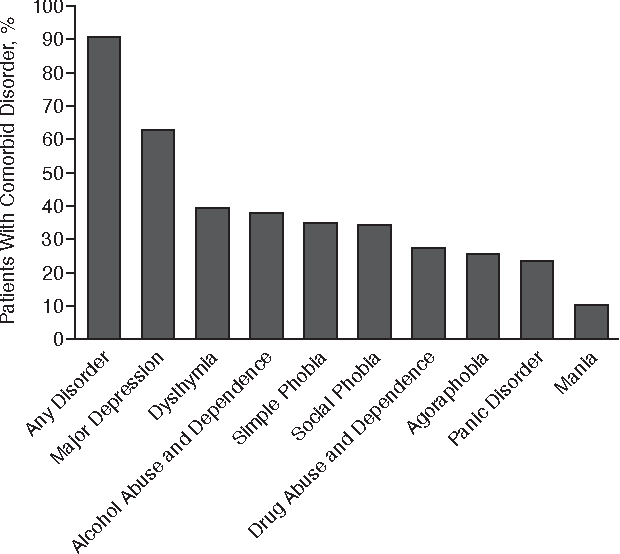
Common Comorbid Disorders Among Bipolar Patients
Bipolar disorder is challenging on its own, but this illness is also likely to be accompanied by certain other physical and mental disorders in a situation known as comorbidity. In these cases, psychiatric treatment may become more complicated and physical interventions may be necessary. Unfortunately, patients who suffer from both bipolar and another disorder may be faced with more obstacles on the road to wellness. Below are some of the most common comorbidities that are seen among bipolar patients.
What Is The Difference Between Bipolar Disorder And Manic Depression
Diagnostic and Statistical Manual of Mental Disorders
It’s also been argued that the older term carries a stigma in popular culture and that both “manic” and “depression” are now used to describe everyday feelings and emotions. As a result, bipolar disorder is now the preferred term and the one that healthcare professionals use in diagnosis.
You May Like: What Causes Anxiety And Panic Attacks