Field Medical Clearance Criteria
To determine if a medical clearance is required for all other patients, EMS personnel are to ask themselves the following questions. If the answer to any of them is yes, the patient should be transported to the nearest, most appropriate receiving facility.
What Happens In Court
If an application for 96 hours is presented to the Probate Division of the Circuit Court, the judge will decide whether to order the person detained, evaluated, and treated in an appropriate facility for up to 96 hours.
If a petition is filed for commitment beyond the initial 96-hour period, a formal hearing will be held in the court to hear facts supporting the petition. During this hearing the person against whom the petition is filed will be represented by an attorney if the person cannot afford an attorney, the court will appoint one. The judge will hear the evidence and make the final decision as to whether the person will be committed for an additional period.
Violence Against Ems Providers
Assault against prehospital providers is pervasive and a significant issue. My colleagues and I completed a study of over 2,500 EMS providers and asked them about their experiences with violent patients. More than 90 percent of field providers have been assaulted or threatened. There are also high rates of sexual harassment against female EMTs and paramedics.
EMS providers need to make their ambulances as safe as possible not just for psychiatric patients, but for any patient. Here are five tips for both field transports and interfacility transfers of psychiatric patients.
Also Check: Schizophrenia Progression
A Typical Protocol Might Follow These Initial Steps Called Zellers Six Goals Of Emergency Psychiatric Care:
- Exclude medical etiologies of symptoms
- Rapidly stabilize the acute crisis
- Avoid coercion
- Treat in the least restrictive setting
- Form a therapeutic alliance
- Formulate an appropriate disposition and aftercare plan
Patients with a potentially life-threatening illness or injury should be transported to the closest, most appropriate receiving hospital for the patients medical needs.
Enlightenment And Modern Era
Schizophrenia continued to be considered âmadnessâ for hundreds of years. Until the mid-20th century, the treatment of schizophrenia was often experimental at best and cruel and inhuman at worst.
McDonough told Psych Central: âIn the beginning, people were considered incurable. They were often locked up in asylums. In Europe, people visited asylums as if they were going to the zoo.
McDonough continued, âBasically, the story is about not seeing human beings as human beings.
Read Also: Paraphobia Meaning
What Is A Psychiatric Disorder
Behavioral and psychiatric disorders are behavioral or mental patterns that cause significant distress or impairment of personal functioning. The condition may be persistent, relapsing and remitting, or occur as a single, isolated episode.
The causes of behavioral disorders are often unclear, but they are usually defined by a combination of how the patient behaves, feels, perceives, or thinks.
Treatment for behavioral and psychiatric disorders can be found in psychiatric hospitals or the community. Assessments are carried out by mental health professionals, such as psychiatrists, psychologists, psychiatric nurses, and clinical social workers, using various methods, including psychometric tests, observation, and questioning.
The two primary treatment methods for psychiatric disorders are psychotherapy and psychiatric medication. Other treatments include lifestyle changes, social interventions, peer support, and self-help. A small number of cases might require involuntary detention or treatment. Prevention programs have been shown to reduce depression.
In 2019, common mental disorders around the globe were:
- Depression
- Delirium
- Dementia
Evaluation And Management Of Psychiatric Emergencies In The Prehospital Setting
Your unit is dispatched to a nearby bus station for a psychiatric disturbance. Upon arrival, you encounter a 61-year-old homeless male, whom youve transported multiple times before for delusions and hallucinations, complaining he has demons in his chest. Hes alert and oriented, very anxious, slightly diaphoretic, breathing heavily and noted to have rapid speech. He yells, Get them out of me! Get the demons out of me!
Prehospital providers will routinely encounter patients with acute psychiatric disturbances and substance intoxication. Further, life-threatening medical conditions may be mistaken for behavioral disturbances. A thorough understanding of the presentation and management of such patients is essential to provide safe and expedient transport to definitive care.
The Suicidal PatientSuicide is the 11th leading cause of death in the U.S., and suicide attempts comprise more than 500,000 ED visits annually.1
Encountering a patient whos attempted suicide or is threatening to attempt suicide can pose many challenges to prehospital providers. As always, scene safety is the first priority. It may be helpful to request law enforcement involvement early to assist in maintaining a safe environment. Its particularly important to ensure the suicidal patient isnt in possession of any potentially harmful items such as weapons, medications or toxic substances, and sharp objects.
References
Also Check: Bpd And Bipolar Comorbid
Excited Delirium Strikes Without Warning
> > Discuss the pathophysiology of excited delirium> > Recognize the signs and symptoms excited delirium> > Identify the treatment for a patient presenting with excited delirium
Key TermsBells Mania: A condition that manifests with mania and fever in which the patient becomes exhausted due to mental excitement.Benzodiazepine: A medication that results in sedative, hypnotic, anxiolytic, anticonvulsant, muscle relaxant and amnesic action. Dissociative agents: Medications that produce a trance-like state by causing interruption of cerebral association pathways between the limbic and cortical systems.Dopamine: A catecholamine neurotransmitter produced in several areas of the brain, including the substantia nigra.Excited delirium: A condition that manifests as a combination of delirium, psychomotor agitation, anxiety, hallucinations, speech disturbances, disorientation, violent and bizarre behavior, insensitivity to pain, elevated body temperature and superhuman strength.Neuroleptic malignant syndrome: A condition that causes delirium and death as a result of abrupt withdrawal from psychiatric medication that blocks dopamine re-uptake.
References
1. U.S. Department of Justice. Study of Deaths Following Electo-Muscular Disruption. www.ojp.usdoj.gov/nij/pubs-sum/222981.htm.
2. Canadian Police Research Centre. Technical Report TR-01-2006 Review of Conducted Energy Devices. www.css.drdc-rddc.gc.ca/cprc/tr/tr-2006-01.pdf.
Managing A Psychiatric Emergency
Psychiatric Times
What Every Psychiatrist Needs to Know to Be Prepared
Psychiatric emergencies encompass situations in which an individual cannot refrain from acting in a manner that is dangerous to himself or herself or to others. The patient may be aware of the danger his behavior poses or he may lack insight into the effects of his actions . Even if the patient perceives that his actions are dangerous, he may be bent on engaging in these behaviors despite the risks. . Because of their lack of insight and judgment, patients in psychiatric emergencies are often brought to the attention of medical professionals by people in the community, including friends, family, police officers, or even bystanders.
Astute psychiatrists may also recognize psychiatric emergencies during routine outpatient care. Patients may report their inability to remain safe, either spontaneously or as elicited by the psychiatrist. When an emergency is recognized, the clinician must:
Perform a complete assessment of the concerning behavior
Reduce risk by transferring the patient to an emergency department or to a psychiatric hospital as needed
Provide or arrange for follow-up for continuity of care
Agitation is a common element in many psychiatric emergencies and poses unintentional danger both to self and to others. Intentional self-endangerment is often accompanied by suicidal ideation. This article will focus on these presentations.
Pre-crisis planning
Also Check: Sex Differences In Depression
A Man In His 50s With Schizophrenia Hypoglycemia And Vague Chest Pain And Shortness Of Breath For A Few Days
The impression that I get from the documentation is that the patient was still felt to be somewhat altered, and the history was felt to be somewhat unreliable and vague. The notes report that the patient has a history of schizophrenia, HTN, diabetes, and atrial fibrillation not on anticoagulation due to noncompliance. At triage, the patient was again able to independently report “shortness of breath” as the chief complaint. His vitals were within normal limits.
His triage ECG at 1741 is shown here:
| What do you think? |
I see atrial fibrillation without any clear signs of ischemia. Borderline low voltage. Even with the baseline ECG available, I don’t see a meaningful change.
A broad workup was ordered, including troponin and head CT.
The head CT showed no acute intracranial abnormality. The patient was given food, and serial fingersticks did not show any further hypoglycemia. All reports continue to describe the patient as “encephalopathic” and a “poor historian,” but all reports also agree that the patient would complain of vague chest pain and shortness of breath when asked.
The initial high sensitivity troponin I returned elevated at 62 ng/L . Due to the elevated troponin, another ECG was ordered at 2036 :
This ECG is importantly and diagnostic different than the first!
These changes were not appreciated, and no more troponins were ordered in the ED. The patient was admitted to medicine.
At 0630 that morning, another ECG was ordered :
| Still obvious STEMI OMI. |
Schizophrenia In The 20th Century
Swiss psychiatrist Eugène Bleuler coined the term âschizophreniaâ in 1900, replacing the term âdementia precociousâ. Bleuler also invented the famous âfour Aâsâ of schizophrenia describing the negative symptoms of schizophrenia, which were later replaced by the 5 Aâs.
Institutionalizing people with schizophrenia was still common practice until the 20th century.
Common 20th century treatments for schizophrenia included:
- insulin therapy for coma: repeatedly injecting large amounts of insulin to induce daily comas over a period of several weeks
- Metrazol shock: a potentially fatal form shock therapy involving injections of Metrazol to trigger seizures and coma
- electroconvulsive therapy: stimulate or shock the brain with electricity to cause seizures
- operation: including frontal lobotomy
Eugenics also played a dark role in treatments for schizophrenia in the 20th century. At the time, schizophrenia was considered a largely hereditary disease. Due to persistent stigma and misunderstanding, many people with schizophrenia have been sterilized, often without consent.
The first antipsychotics, such as Chlorpromazine, were developed and marketed in the 1950s. The availability of these drugs and similar drugs led to widespread deinstitutionalization in the 1960s. These drugs are still prescribed today and are considered to be âtypical antipsychoticsâ.
- Communication disorders index
- The Positive and Negative Symptom Scale
- BPRS
- The mini mental state examination
Read Also: What Is Pristiq Used For
Learn How Emts & Paramedics Identify Treat And Care For Patients With Behavioral And Psychiatric Emergencies
Behavioral and psychiatric disorders are the fifth most common emergency that EMS professionals respond to, accounting for almost 8% of all EMS calls.
Behavioral and psychiatric disorders are behavioral or mental patterns that cause significant distress or impairment of personal function.
A behavioral or psychiatric disorder is defined by the patient showing any of the following signs:
- Is a danger to themselves
- Is a danger to others
- Is so mentally impaired that they cannot provide for their own food, clothing, or shelter
- Appears at risk to evolve into one of the above conditions
Mental illness can sometimes be associated with aggressive or violent behavior. However, people living with a mental illness and receiving effective treatment are no more violent or dangerous than the rest of the population. People living with a mental illness are more likely to harm themselvesor be harmed than to hurt other people.
Violence is not a symptom of psychiatric illness. The relationship between mental illness and violence is complex. Research suggests there is little relationship between mental illness and violence unless substance use is involved.
For current or aspiring EMS professionals, this post discusses the pre-hospital treatment for behavioral and psychiatric disorders, one of the most common emergency calls for EMTs and paramedics.
How To Make 911 Respond To Your Calls
Also see this excellent info from NAMI Glendale, CA. /
Individuals with neurobiological disorders are occassionaly danger to themselves, suicidal and/or danger to others. When this happens, you may want to call 911. It is often difficult to get 911 to respond to your calls if you need someone to come & take your MI relation to a hospital emergency room . They may not believe that you really need help. And if they do send the police, the police are often reluctant to take someone for involuntary commitment. That is because cops are concerned about liability. They dont want to be sued for taking someone to the ER involuntarily. Another reason is that they must stay with the person until he or she is admitted. This can take between 2-48 hours. Cops dont want to sit in ER sergeants dont want to take two police off the streets.
Following is how you can make 911 & the police overcome their reluctance to help.
When the police come, they need compelling evidence that the person is a danger to self or others before they can involuntarily take him or her to ER for evaluation. If the person stops acting out by the time police arrive, this can be difficult. Again, give specific recent examples of danger.
911 should be first resort in an immediate emergency, & the last resort when its not. If your family member needs help, not necessarily hospitalization, try Mobile Crisis Intervention Services.
Read Also: Dehydration Causes Anxiety
Treatment Guidelines & Resources For Medical First Responders
Treatment guidelines for behavioral and psychiatric emergencies can be found on page 53 of the National Model EMS Clinical Guidelines by the National Association of State EMT Officials . NASEMSO maintains these guidelines to facilitate state and local EMS system clinical guidelines, protocols, and operating procedures. These guidelines are either evidence-based or consensus-based and have been formatted for use by EMS professionals.
The guidelines include a rapid assessment of the patient for symptoms of psychiatric disorder, which may include:
EMS providers should reference the CDC Field Triage Guidelines for decisions regarding transport destination for injured patients.
Background: Extent And Description Of The Problem
The incidence of suicide surpasses homicide and is the eighth leading cause of death in the United States. About 1% of total deaths are a result of suicide. Unsuccessful attempts outnumber completed suicides by a multiple of 16.1 It has been estimated that the average number of suicide attempts in a family practice is 10 to 15 yearly, although the family physician may be aware of only 1 or 2.2 Multiple attempts are more likely to occur in the adolescent and young adult age groups. Frequently, the geriatric patient who commits suicide has not made previous attempts.3
Differentiation between a suicide attempt and a parasuicide has been suggested.4 Parasuicide refers to an act of self-harm without the realistic expectation of death. These behaviors have also been referred to as suicidal gestures and viewed as different from a true attempt in which there is a clear intent and expectation of death. However, gestures can also lead to death when there are miscalculations or unexpected effects of the harmful behavior. In addition, it is difficult and sometimes impossible to discern accurately the patient’s intent. As a result, parasuicides or gestures should be taken seriously and deserve the same intensive intervention as unambiguous suicide attempts.
Managing the patient who has attempted suicide requires a comprehensive plan. The algorithm in Figure 1 describes an overall assessment and management strategy. The following sections detail the recommended steps.
You May Like: What Is The Phobia Of Puke Called
Restraint And Sedation Protocols
All EMS providers should have clear protocols that allow for patient restraint and sedation. Indeed, it is incumbent on ALS providers to keep hospital staff safe by adequately sedating the patient before arrival at the emergency department.
EMS systems and providers are sophisticated enough to handle a wide variety of patients, psychiatric and otherwise. Ambulances can be made safe by the providers who work in them. EMS system administrators, chiefs and other stakeholders need to insist on training for psychiatric patient treatment and transport.
References
1. Elbogen EB Johnson SC The Intricate Link Between Violence and Mental Disorder. JAMA Psych. 2009 66:152-161.
2. O’Connor v. Donaldson, 422 U.S. 563 .
3. Dunn TM Johnston JW Dunn WW Doty C. Assaults Against EMS Providers. Presentation to 26th Annual Meeting of the Association for Psychological Science, San Francisco, 2014.
About the Author
Dr. Thomas Dunn is an Associate Professor of Psychological Sciences at the University of Northern Colorado. He earned a Ph.D. in clinical psychology and clinical neuropsychology in 1999. Dr. Dunn is on faculty at Denver Health Medical Center as a licensed psychologist and is a member of its ethics committee. Thom also has 25 years of experience in EMS having worked in a number of EMS settings including backcountry rescue, fire-based EMS, and is presently a paramedic field instructor for Denver Paramedics, the 911 provider to the city and county of Denver, Colorado.
Thank You!
Excited Delirium And The Dual Response
Preventing In-Custody Deaths
Excited delirium syndrome is a serious and potentially deadly medical condition involving psychotic behavior, elevated temperature, and an extreme fight-or-flight response by the nervous system. Failure to recognize the symptoms and involve emergency medical services to provide appropriate medical treatment may lead to death. Fatality rates of up to 10 percent in ExDS cases have been reported.1 In addition to the significant morbidity and mortality associated with unrecognized ExDS, a substantial risk for litigation exists. These patients often die within 1 hour of police involvement. One study showed 75 percent of deaths from ExDS occurred at the scene or during transport.2 Law enforcement organizations should take steps to increase officer awareness of ExDS and its symptoms and develop procedures to engage the medical community when identified. Without placing themselves or others at a greater risk for physical harm, officers must be able to rapidly detect symptoms of ExDS and immediately engage EMS for proper diagnosis and medical treatment. Failure to do so may prove fatal.
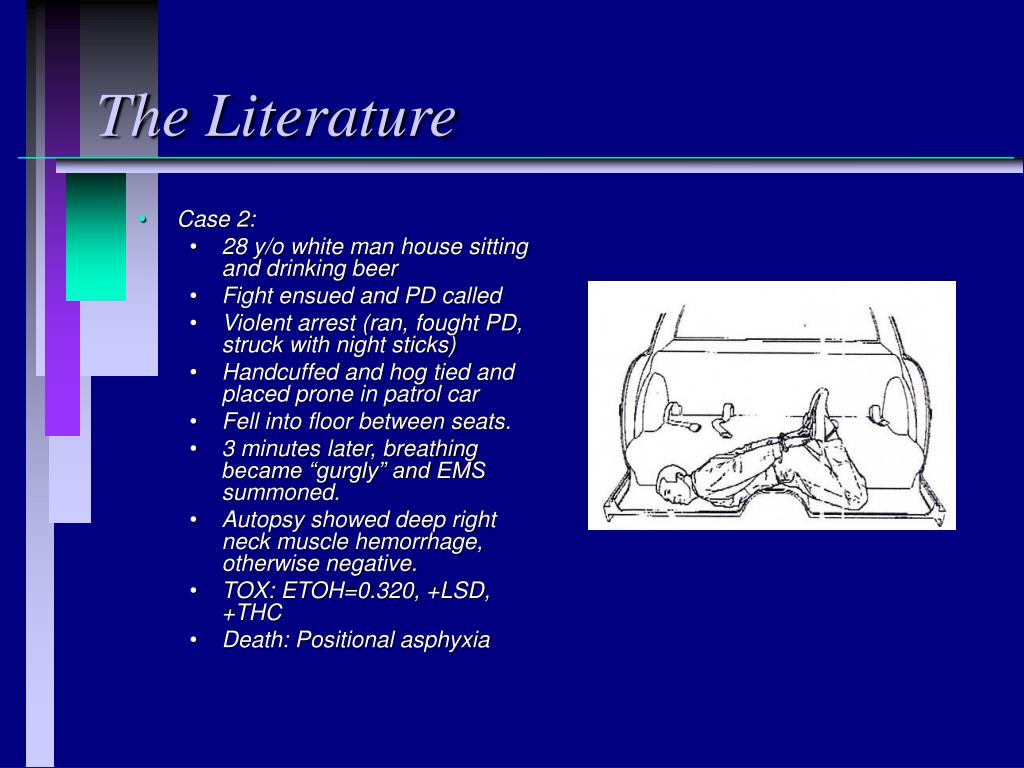
Historical Data and Cases Reviewed
Dr. Roach is a 2014 graduate of the Department of Emergency Medicine residency at Regions Hospital in Saint Paul, Minnesota.
Dr. Echols is a 2014 graduate of the Department of Emergency Medicine residency at Regions Hospital in Saint Paul, Minnesota.
Medical Background
Table 1
Risk Factors Associated with Excited Delirium Syndrome
Also Check: Aphobic Meaning