Parkinsonian And Other Extrapyramidal Features In Antipsychotic
If involuntary movements are indicative of dysfunction in the extrapyramidal motor system and implicate basal ganglia disease, the question arises as to whether other signs of extrapyramidal dysfunction, such as Parkinsonism, may also be intrinsic to the disease process of schizophrenia.
Although the historical literature noted similarities between some clinical characteristics of schizophrenia and Parkinsonism, Caligiuri et al published the first contemporary report of Parkinsonism in antipsychotic-naive patients: clinical evaluation of 24 newly diagnosed patients with schizophrenia revealed 21% to evidence rigidity and 12% bradykinesia, while quantitative methods revealed 29% to evidence rigidity and 37% tremor the same quantitative methods indicated 4% of controls to evidence rigidity in the absence of other extrapyramidal features.
These findings extend the concept of movement disorder in untreated schizophrenia, through involvement not just of involuntary movements but also of Parkinsonian features, as an intrinsic component of a disease process involving dysfunction in basal ganglia-cortical mechanisms.
How Does A Patient Recover
Patients can recover from acute episodes. They will begin to stabilize when they take medications that control their symptoms. After that, they may still have some trouble with symptoms, but these will be much less severe. Between episodes, maintenance is important to prevent mild and persistent symptoms. During this phase, many patients continue to improve.
How Does The Classification Process Work
The World Health Organization classifies diseasesincluding neurological conditionsthrough the International Classification of Diseases . Once this organization approves a new ICD revision, it is submitted to the World Health Assembly for approval. In the United States, the Centers for Disease Control and Preventions National Center for Health Statistics implements the ICD through diagnosis codes used for billing by physicians.
Don’t Miss: Can You Go To Urgent Care For Panic Attacks
Health Advocates Say Schizophrenia Should Be Reclassified As A Brain Disease
Changing the definition could unlock more money for cures.
Mental health advocates are lobbying Congress to help them get schizophrenia classified as a brain disease like Parkinsons or Alzheimers, instead of as a mental illness, a move that could reduce stigma and lead to more dollars for a cure.
Federal health officials, scientists and doctors say conditions that cause psychosis, such as schizophrenia and bipolar disorder, are poorly understood and, in the public mind, often associated with violent behavior. Patients are more likely to be homeless, incarcerated, commit suicide and die younger than those with any other neurological diseases.
Look at the disconnect in the way these patients are treated. Its unconscionable, said Raymond Cho, professor of psychiatry research at Baylor College of Medicine and chairman of the Schizophrenia and Related Disorders Alliance of America.
His group is among those focusing on appropriators in Congress particularly those who have championed mental health in the past to include schizophrenia in a new CDC program that aims to collect data on the prevalence and risk factors of neurological conditions in the U.S. population. The findings could eventually be used to push the World Health Organization to reclassify the disorder a complicated process that may take years.
The problem is the CDC only has enough money to study a finite number of conditions, putting disease advocacy groups in competition with each other.
Specificity Of Spontaneous Dyskinesia To Schizophrenia
Spontaneous involuntary movements in the healthy and thus unmedicated elderly are relatively infrequent, with a prevalence of 1%8% however, both prevalence and severity rise considerably with a diversity of organic brain disorders that are not common indications for antipsychotic treatment., In the only systematic, comparative study, a higher prevalence of spontaneous involuntary movements was reported in untreated schizophrenia vis-à-vis nonpsychotic patients having primarily affective and personality disorders.
Read Also: Pristiq For Bipolar
Crossley Et Al’s Meta
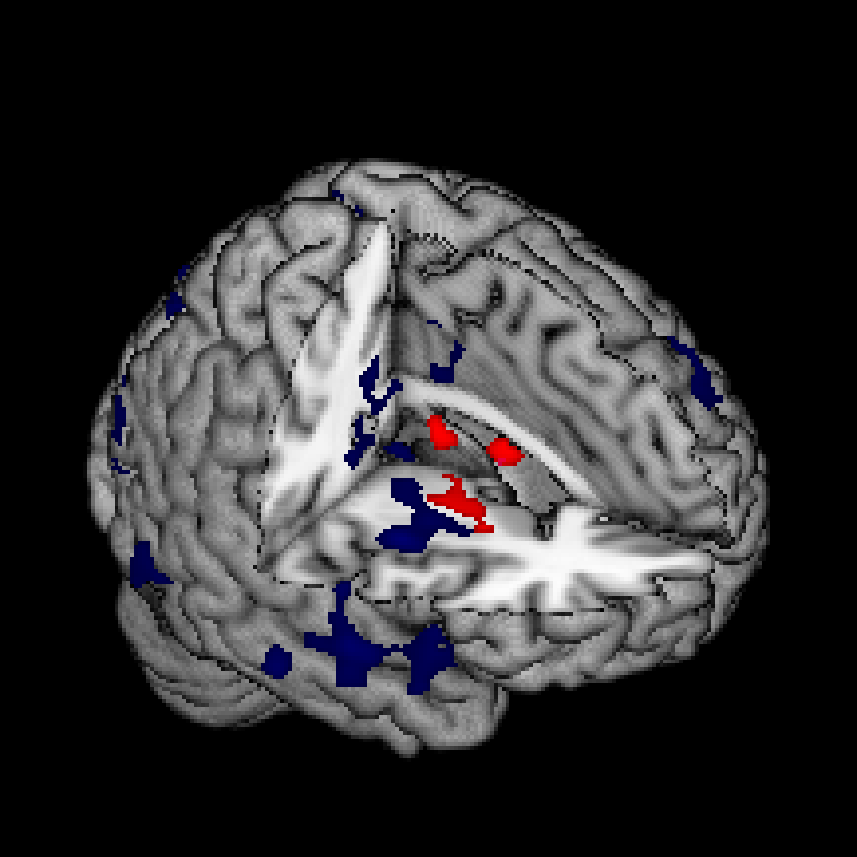
The paper by Crossley and colleagues takes a novel approach.Reference Crossley, Scott, Ellison-Wright and Mechelli1 It is a meta-analysis of studies using voxel-based morphometry tomeasure changes in grey matter in neurological and psychiatric diagnosticgroups. So there are studies of diseases as diverse as multiple sclerosis andHuntington’s disease, Asperger syndrome, anorexia and Alzheimer’s disease,schizophrenia and panic disorder, each comparing a patient group with controlsand reporting statistical differences in, strictly speaking grey matter densityused as a proxy for volume change, usually with, areas of reduced grey mattermapped onto a brain template. Importantly, these methods look at the wholebrain and are not influenced by prior assumptions of where the abnormalitymight be. The authors applied some basic quality controls over the includedstudies and applied weightings according to the numbers of participants butwere interested in the broad pattern that such large data-sets mightreveal.
Conditions That Can Seem Like Schizophrenia
Schizophrenia is a mental illness that affects how you think and behave. The symptoms of schizophrenia include:
- Psychotic symptoms including hallucinations, hearing voices, or believing someone or something is out to get you
- Negative symptoms such as a lack of interest or an inability to take pleasure in daily activities and spending time with others
- Cognitive symptoms including trouble focusing and making decisions
Many of the symptoms of schizophrenia are also symptoms of other conditions. Because of this, people often get misdiagnosed.
Other disorders and conditions that are sometimes mistaken for schizophrenia include:
Schizoaffective disorder. Schizoaffective disorder causes many of the symptoms of schizophrenia, like delusions. But people with schizoaffective disorder also have periods of depression or periods where they feel extremely energized or happy . Thatâs not usually the case with schizophrenia.
Schizoid personality disorder. A person with schizoid personality disorder avoids social situations and interacting with others. They usually have a hard time feeling and expressing emotions. Even though schizoid personality disorder sounds a lot like schizophrenia, people who have schizoid personality disorder donât have delusions or hallucinations.
Recommended Reading: Does Pristiq Help With Anxiety
Why Should Schizophrenia Be Classified As A Neurological Disease
Reclassifying schizophrenia as a neurological disease makes sense for a number of reasons.
The defining feature of schizophrenia is psychosis, manifested primarily by delusions and hallucinations associated with structural and chemical changes in the brain. Psychosis symptoms are also found in dementia, Parkinsons disease, strokes, and brain tumorsall of which are also characterized by structural and chemical changes and classified as nervous system disorders.
Auditory hallucinations or delusions are not simply a behavioral problem, and any clinician with experience treating schizophrenia will recognize how a patients thoughts, emotions, and behaviors are hijacked by a biological process beyond their control.
In the lab, many genetic, post-mortem, and neuroimaging studies have demonstrated clear evidence of schizophrenias biological underpinnings. For example, if one twin in an identical pair has schizophrenia, the other has a 50% chance of also developing the illness, even if the second child was raised in a different environment. This number is comparable to that for Alzheimers disease and greater than that for Parkinsons disease.
Can The Brain Look Normal In Schizophrenia
The teams resulted identified a split in their patients that surprised the authors. Numerous other studies have shown that people with schizophrenia have significantly smaller volumes of brain tissue than healthy controls. However, for at least a third of patients we looked at, this was not the case at all — their brains were almost completely normal,” said Davatzikos in a press release.In the reduced volume group, patients brains showed significantly less brain matter than seen in healthy controls across several brain regions including the thalamus and frontal cortex. In the second subtype, the only differences noted were an increased amount of gray matter consisting mainly of neurons in the basal ganglia, a brain area linked to motor control, and a higher white matter consisting of axonal connections volume in deeper brain areas.
Read Also: What Is The Phobia Of Storms Called
Future Research On Neurological Signs
At present, most of the scales used to measure NSS were devised using nonfirst-episode cases, and no scales have been validated in antipsychotic-naive first-episode samples. Similarly, in the case of one of the most widely used scales , the various subscales have not been validated in first-episode samples. Two studies, validated subscales in nonfirst-episode samples, and similar studies of first-episode patients would further validate the conceptual categories of NSS that are widely used today. Some of the inconsistency in findings across studies could be accounted for by the different scales used to measure NSS, with some scales more likely to be influenced by changes in mental state while others focus more on harder signs that tend not to show the same degree of variation over time. Future research should further validate the assessment scales used in first-episode samples, and harder signs should be included as standard in each assessment of NSS.
Neurological Signs And Antipsychotic Medication Variables
Antipsychotic treatment often causes the emergence of extrapyramidal symptoms and/or tardive dyskinesia . These motor symptoms may be erroneously rated as neurological signs. The demonstration that SNS are independent of antipsychotic treatment or side effects would support the hypothesis that neurological signs are related to disease etiopathophysiology and an overt manifestation of the brain impairment resulting in schizophrenia.
Also Check: What Are The Three Stages Of Schizophrenia
What Can I Expect From Schizophrenia
If you have schizophrenia, you should know that the course of this brain disease varies greatly. Medication can often control your symptoms. If you take your medication exactly as directed, you will likely have a mild type of the disease. In that case, you will have only one or two relapses in total by the age of 45 and will show only minor symptoms. If you have moderate schizophrenia, you will likely have several major relapses by the age of 45, plus symptoms during stressful times, and you will have persistent symptoms between relapses. This often results from taking your medication most, but not all, of the time. Not taking medication at all or dropping out of treatment often causes a severe and unstable course of the disease. If you have this type, you will only be stable for a short period of time between relapses. You may have serious symptoms and need help with your day-to-day life.
Should Patients Take Medication During Recovery

Researchers have not found a cure for schizophrenia, so it is important to take any medications prescribed as they are given. The symptoms of schizophrenia can be controlled in most people as long as they take their medications. After the first episode, doctors recommend that patients stay on medication for 12 to 24 months before reducing the dose. Patients who have had more than one episode or those who have not fully recovered may need to be treated for a longer period of time, and some people may need treatment indefinitely.
Patients need to be careful and recognize side effects of medications, since some can cause fairly large problems. Extrapyramidal side effects can cause people to feel rigid or stiff, or they may feel like they need to keep moving all the time. Doctors may prescribe an anticholinergic in some cases to help treat this side effect. People can also develop tardive dyskinesia when they take antipsychotics for a long period of time. This results in the uncontrolled movement of the mouth. If this develops, simply switching the type of antipsychotic can help.
For more on the topic of Schizophrenia , weve included the following expert consensus documents as reference materials:
Also Check: Phobia Meaning In English
New Strong Evidence For Neurological Cause Of Schizophrenia
A team of scientists claims to have finally started to understand what goes wrong in schizophrenia, following the discovery that disease-linked mutations disrupt genes responsible for maintaining a chemical balance in the brain crucial for healthy brain development and function
The mutations disrupt genes that regulate excitatory and inhibitory neurotransmission, which needs to be delicately balanced to ensure the brain functions properly.
Our study marks a significant step towards understanding the biology underpinning schizophrenia, which is an incredibly complex condition and has up until very recently kept scientists largely mystified as to its origins, says lead author Dr. Andrew Pocklington of Cardiff University, Wales.
We now have what we hope is a pretty sizable piece of the jigsaw puzzle that will help us develop a coherent model of the disease, while helping us to rule out some of the alternatives. A reliable model of disease is urgently needed to direct future efforts in developing new treatments, which havent really improved a great deal since the 1970s.
Experts have known for some time that schizophrenia is a highly heritable disorder. While schizophrenia occurs in 1% of the general population, it occurs in 10% of people who have a first-degree relative with the condition. The identical twin of someone with schizophrenia has a 40-65% chance of developing the disorder themselves.
Evidence That Schizophrenia Is A Brain Disease
Data from modern scientific research proves that schizophrenia is unequivocally a biological disease of the brain, just like Alzheimer’s Disease and Bipolar Disorder. For one thing, schizophrenia is now known to be partially caused by genetics and to be inherited. For another, modern non-invasive brain imaging techniques such as Magnetic Resonance Imaging and Computerized Tomography , have documented structural differences between schizophrenic and normal brains. Individuals with schizophrenia have up to 25% less volume of gray matter in their brains, especially in the temporal and frontal lobes . Patients demonstrating the worst brain tissue losses also tend to show the worst symptoms.
Functional scanning of the brain, using technologies like Positron Emission Tomography and functional MRI have made it possible to create real-time maps of regional cerebral blood flow and metabolism, providing another window into how schizophrenic brains are distinct from normal brains. Such studies tend to show low levels of activation in schizophrenic patients’ middle frontal cortex and inferior parietal cortex compared to normal people included as control subjects. Low activity findings like this are also correlated with increased negative symptoms .
Considered as a whole, these numerous and methodologically distinct results suggest converging and compelling evidence for the idea that schizophrenia is basically a biologically based brain disease.
Recommended Reading: What Is The Phobia Of Throwing Up
Mental And Neurological Disorders
Over the past 50 years, pharmaceutical innovation has contributed to transforming mental and neurological disorders from highly-stigmatized and poorly-understood diseases into treatable and often curable conditions.
Reducing the burden of mental and neurological disorders relies on both timely diagnosis and the treatment of disorders by health professionals through pharmacological and psychosocial interventions. Furthermore, successful screening relies on reducing stigma and better integrating health services.
The World Health Organization estimates that 700 million cases of mental and neurological disorders are reported annuallyaccounting for 13% of global disease burden. Out of this number, 150 million people live with depression, 25 million live with schizophrenia, 38 million live with epilepsy, and 90 million live with a substance abuse disorder. A number of factors are responsible for increasing the disease burden: insufficient focus on basic mental health care, lack of funding of prevention programs, and the stigma associated with these disorders. The costs to society in terms of worker disability call for urgent action and coordinated efforts from all health partners to reverse current trends.
The brain is a uniquely complex organ and research in this area is very difficult, expensive, and time-consuming. Developing new medicines for MNDs and bringing them to market takes longer and is more expensive than developing medicines for other serious disorders.
Clinical Features Of Schizophrenia
Schizophrenia affects about 1% of the worlds population, .
Symptoms of schizophrenia may include hallucinations and delusions . These symptoms are referred to as positive symptoms though they are not positive to the person experiencing them. These symptoms are attributed to an increased activity of the neurotransmitter dopamine in a certain region of the brain.
Withdrawal, lack of interest in things a person used to love, or loss of interest in self-care, such as not eating or showering, are commonly called negative symptoms of schizophrenia. Some of these symptoms are known to be associated with a reduction of the same neurotransmitter dopamine in the frontal region of the brain, affecting the ability to be motivated, display normal facial expressions, or to initiate an action. Cognitive impairment is another important set of symptoms including memory deficits and inability to plan or make decisions. Furthermore, patients suffering from schizophrenia often do not realize they are sick and resist being hospitalized or refuse medications that can help them. The lack of insight in schizophrenia is quite common in schizophrenia. Medications as well as counselling can help patients develop awareness that they do have a medical illness and that they should adhere to their medication in order to achieve remission and ultimately recovery.
Also Check: Is Tequila A Stimulant
Why Does Reclassification Matter
We believe reclassifying schizophrenia as a neurological disease is an important first step to providing better care. Our strategy is designed to measure the total societal burden of schizophrenia in the United States, including healthcare costs, criminal justice system and social welfare system costs, impacts of unemployment and underemployment, and impacts on caregivers.
Understanding the full impacts of schizophrenia on those living with the disease and on society is critical to providing supportive evidence for reclassification.
Additionally, S& PAA plans to leverage the findings from this research to address health inequities caused by the inappropriate classification and subsequent inappropriate care system for those living with the disease. Findings will be used to motivate policy changes to improve access to affordable and appropriate health care and related services including, but not limited to:
- Providing increased access to appropriate treatment by a comprehensive, integrated team of encompassing psychiatrists, neurologists, and other providers
- Building on the Helping Families in Mental Health Crisis Act by continuing to expand access to public and private psychiatric hospitals through exceptions to the Medicaid Institution for Mental Diseases exclusion
- Double federal appropriations for the Assisted Outpatient Treatment program administered by the Substance Abuse and Mental Health Services Administration