Bipolar Disorder And Substance Abuse Can Go Hand In Hand
Substance abuse often complicates the diagnosis and treatment of bipolar disorder. Substance abuse is bipolar disorders partner in crime. Some studies show that as many as 60% of people with bipolar disorder also abuse drugs or alcohol. Untreated substance abuse can make it virtually impossible to manage the mood symptoms of bipolar disorder if both disorders are present. It can also be hard to make a confident diagnosis of bipolar disorder when someone is actively abusing substances that cause mood swings.
Substances such as alcohol and cocaine can also cloud the picture in bipolar disorder. For example, people high on cocaine can appear manic when theyre actually intoxicated,Ã or have a depression crash when the drug wears off. Some people with bipolar disorder use drugs and alcohol as a part of the impulsivity and recklessness of mania. Others may have an independent substance use disorder, which requires its own treatment. Substance abuse may make bipolar episodes more frequent or severe, and medicines used to treat bipolar disorder are usually less effective when someone is using alcohol or illicit drugs.
Its Similar To Other Mental Health Conditions
People with bipolar disorder usually get diagnosed with something else firstdepression and ADHD are some of the most common. Depression is a part of bipolar disorder, and most people are more familiar with what depression looks like than mania. ADHD can also look very similar to bipolar disorder, especially in children.
Once a person discovers they have bipolar disorder, that might replace any previous diagnosisor they might have multiple mental health conditions at once. If you know someone who is being treated for a mental illness, but they still struggle with symptoms of bipolar disorder, its worth considering that there may be more going on.
What Are Other Types Of Psychotic Disorders
Mental disorders associated with symptoms of psychosis are known as psychotic disorders. In addition to schizophrenia, other psychotic disorders include:
- Schizoaffective disorder:Symptoms of this disorder may include hallucinations, delusions, and disorganized thinking, along with either a depressed or manic mood.
- Schizophreniform disorder:With this disorder, a person develops the symptoms of schizophrenia for a period shorter than six months.
- Delusional disorder:This describes strong, unchangeable beliefs in things that are not real or true, without experiencing hallucinations.
- Brief psychotic disorder:This describes psychotic symptoms with a sudden onset, lasting one month or less. Another episode may or may not occur in the future.
- Substance-induced psychotic disorder: This describes psychosis brought on by the use of substances such as cannabis, cocaine, ecstasy, and alcohol.
- Psychotic disorder due to a medical condition:This describes conditions such as brain tumors, brain infections, or strokes that can lead to psychotic symptoms.
Psychosis can be limited to one episode. However, it is possible to have recurring episodes as part of certain conditions.
Recommended Reading: Feretrophobia Definition
What Are The Symptoms Of Schizophrenia And How Is It Diagnosed
How is schizophrenia diagnosed?
Only a psychiatrist can diagnose you with schizophrenia after a full psychiatric assessment. You may have to see the psychiatrist a few times before they diagnose you. This is because they need to see how often you are experiencing symptoms.
There are currently no blood tests or scans that can prove if you have schizophrenia. So, psychiatrists use manuals to diagnose schizophrenia and other mental illnesses.
The 2 main manuals used by medical professionals are the:
- International Classification of Diseases which is produced by the World Health Organisation , or
- Diagnostic and Statistical Manual which is produced by the American Psychiatric Association .
NHS doctors use the ICD-10.
The manuals explain which symptoms should be present, and for how long for you to receive a diagnosis. For example, according to the NHS you need to be hearing voices for at least 1 month before you can be diagnosed. Mental health professionals may say you have psychosis before they diagnose you with schizophrenia.
What is the future of diagnosis in schizophrenia?There are many research studies being conducted across the world on how to better diagnose schizophrenia. For example, a recent study found through looking at images of the brain, there may be different sub-types of schizophrenia.
What are the symptoms of schizophrenia?
The symptoms of schizophrenia are commonly described as positive symptoms or negative symptoms. This doesnt mean that they are good or bad.
Health Solutions From Our Sponsors
Molecular PsychiatryDiagnostic and Statistical Manual of Mental Disorders, Fifth EditionDiagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text RevisionIndian Journal of PsychiatryPsychiatric ServicesClinical Child Psychology and PsychiatryPsychiatric TimesFrontiers in PsychiatryPsychiatry ResearchJournal of the American Medical AssociationBritish Journal of PsychiatryAmerican Academy of Social Work and Social WelfareScience DailyClinical NeuropsychiatryCurrent Antipsychotics, Handbook of Experimental Pharmacology, Vol. 212Molecular PsychiatryPsychiatria DanubinaSchizophrenia BulletinBritish Journal of PsychiatryScienceSocial Studies of ScienceThe British Journal of PsychiatryAmerican Journal of PsychiatryPatient CareAm J PsychiatryMen and MasculinitiesHistory of PsychiatrySchizophrenia Research TreatmentGerman Journal of PsychiatryLancetPsychiatric ServicesCurrent Opinion in PsychiatryEpidemiologic ReviewsPsychiatric ServicesNeuropsychopharmacology: The Fifth Generation of Progress, Fifth EdClinical Schizophrenia and Related PsychosesPsychological BulletinSchizophrenia ResearchClinical TherapeuticsHarvard Mental Health LettAmerican Journal of PsychiatryAmerican Journal of PsychiatrySchizophrenia BulletinJournal of PsychopharmacologySchizophrenia BulletinAmerican Journal of PsychiatryPsychiatric TimesSchizophrenia BulletinAutismAmerican Journal of Psychiatry
Also Check: Mediocre Medical Symptoms Of Anxiety
The Following Are Some Signs Of Worsening Schizophrenia:
- Disorganized speech: If the person with schizophrenia is speaking in a jumbled or incoherent manner, this could indicate that their medication needs to be adjusted or that they are experiencing a relapse of their illness.
- Reduced or increased social contact: If the person with schizophrenia becomes less social or more isolated this may be a sign that they are slipping back into old patterns of behavior. On the other hand, if they become too attached to a specific individual it could mean that they are developing a new delusion and need to speak to their doctor about adjusting their medication.
- Changes in appetite or weight: If the person with schizophrenia starts overeating and putting on weight, it could be a sign that they are experiencing negative symptoms related to their illness . On the other hand, if they start losing interest in food and begin losing weight, they may be experiencing hallucinations related to food.
- Changes in sleeping patterns: If the person stops sleeping for long periods of time every day, it could be due to their schizophrenia medication interfering with the quality of their sleep. An increase in nightmares or difficulty falling asleep are also common signs of schizophrenia worsening.
What The Research Says
A recent study looked at 114 people with bipolar disorder and stable moods. All of the study participants were being treated with mood stabilizers as opposed to antipsychotics or antidepressants.
The researchers found that people who took the anticonvulsants valproate or lamotrigine had better sexual function scores than people who took lithium or a combination of lithium and benzodiazepines.
In comparison with people who took anticonvulsants alone:
- People who took lithium or a combination of lithium and benzodiazepines had worse sexual desire.
- People who took lithium had worse sexual arousal.
- People who took a combination of lithium and anticonvulsants, or lithium and benzodiazepines had worse sexual orgasm.
Don’t Miss: Phobia Of Puking
First Episode Of Psychosis
The first episode of psychosis refers to when you first show signs of being unable to distinguish whats real from what isnt. It typically involves hallucinations and delusions, which can seem very real to the person experiencing them.
Experts say the average age at which people first experience psychosis is 24 years old. The oldest age of onset was 63 years and the youngest age was 3 years.
Acting quickly to connect yourself or your loved one with the right treatment during early psychosis can help dramatically. If you are a family member or friend, consider reaching out to a healthcare professional on behalf of the person you care about.
Schizophrenia: The 7 Keys To Self
Seek social support. Friends and family vital to helping you get the right treatment and keeping your symptoms under control. Regularly connecting with others face-to-face is also the most effective way to calm your nervous system and relieve stress. Stay involved with others by continuing your work or education. If thats not possible, consider volunteering, joining a schizophrenia support group, or taking a class or joining a club to spend time with people who have common interests. As well as keeping you socially connected, it can help you feel good about yourself.
Manage stress. High levels of stress are believed to trigger schizophrenic episodes by increasing the bodys production of the hormone cortisol. As well as staying socially connected, there are plenty of steps you can take to reduce your stress levels. Try adopting a regular relaxation practice such as yoga, deep breathing, or meditation.
Get regular exercise. As well as all the emotional and physical benefits, exercise may help reduce symptoms of schizophrenia, improve your focus and energy, and help you feel calmer. Aim for 30 minutes of activity on most days, or if its easier, three 10-minute sessions. Try rhythmic exercise that engages both your arms and legs, such as walking, running, swimming, or dancing.
You May Like: Does Pristiq Work For Anxiety
What Are The Signs And Symptoms
A person with bipolar disorder will go through episodes of mania and at other times experience episodes of depression . These arent the normal periods of happiness and sadness that everyone experiences from time to time. Instead, the episodes are intense or severe mood swings, like a pendulum that keeps arcing higher and higher.
Symptoms of mania include:
- anger, worry, and anxiety
- thoughts of death or suicide
In adults, episodes of mania or depression usually last for weeks or months, although they can be shorter in length. In children and adolescents, though, these episodes can be much shorter, and a kid or teen can even go back and forth between mania and depression throughout the day.
Episodes of mania or depression may happen irregularly and follow an unpredictable pattern or they may be linked, with a manic episode always following a period of depression, or vice versa. Sometimes episodes have a seasonal pattern. Mania in the spring, for example, may be followed by depression in the winter.
Between episodes, someone with bipolar disorder usually returns to normal functioning. For some people, though, there is little or no break period between their cycles. These mood swing cycles can change slowly or rapidly, with rapid cycling between mania and depression being much more common in women, children, and adolescents.
P
Family Education And Support
Educational programs for family members, significant others, and friends offer instruction about schizophrenia symptoms and treatments, and strategies for assisting the person with the illness. Increasing key supporters understanding of psychotic symptoms, treatment options, and the course of recovery can lessen their distress, bolster coping and empowerment, and strengthen their capacity to offer effective assistance. Family-based services may be provided on an individual basis or through multi-family workshops and support groups. For more information about family-based services in your area, you can visit the family education and support groups page on the National Alliance on Mental Illness website.
Don’t Miss: Definition Phobia
Does Schizophrenia Get Better As You Get Older
Schizophrenia does not typically get better as you get older. The symptoms of schizophrenia may become worse over time, or they may remain the same for some people. Schizophrenia is a chronic illness that can be managed with medication and therapy, but it does not typically go away as you get older.
The Signs Of Schizophrenia In Your Early 20s
4 min Read Time
The good news is that with comprehensive treatment and support, most patients can manage their condition effectively.
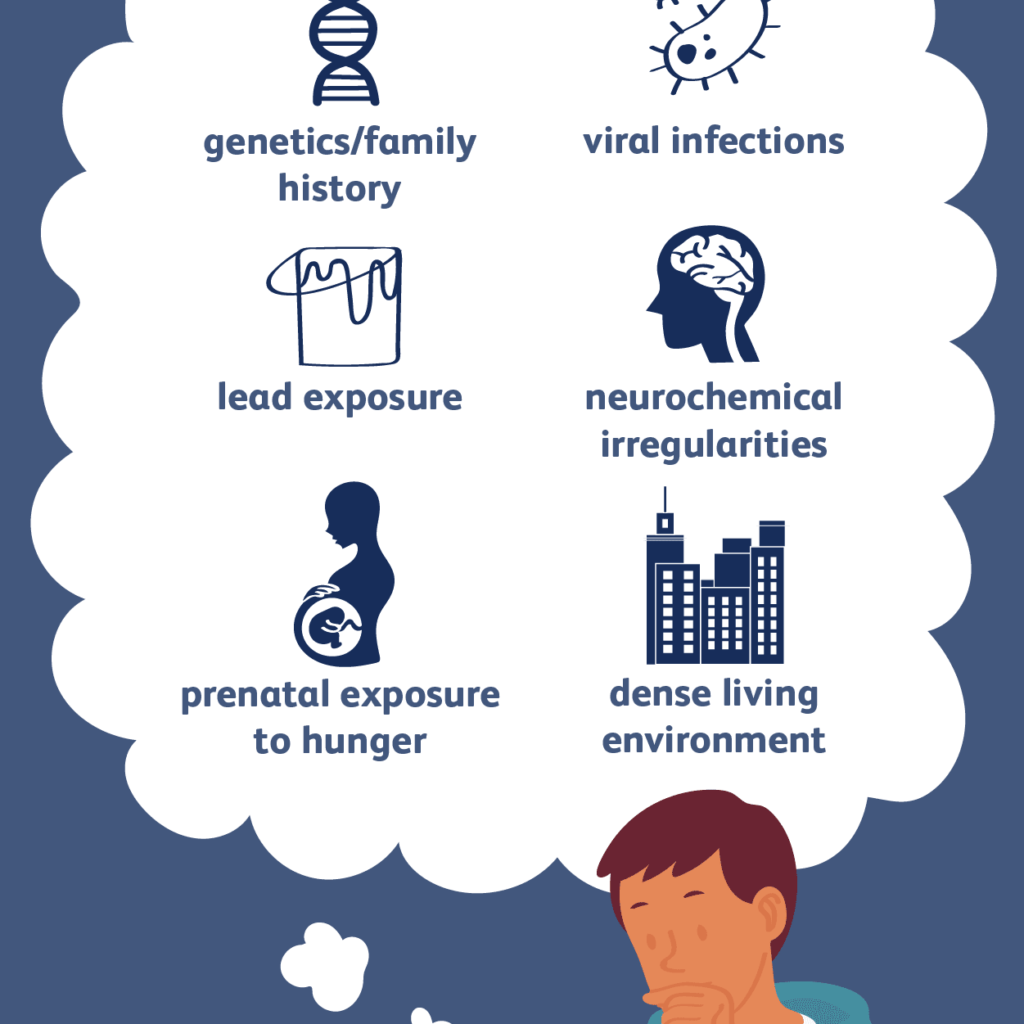
Schizophrenia is a mental disorder characterized by fragmented thoughts and a distorted perception of reality. There is currently no cure. While the origins of the disease are still unclear, researchers believe that it’s likely caused by a combination of genetic and environmental factors.
Also Check: Hippopotomonstrosesquipedaliophobes.
How You Get A Diagnosis
If you or someone you love shows any of these signs, see a doctor right away. The symptoms of prodrome are subtle and easy to miss. Many also overlap with other mental health issues, like depression and substance misuse.
To rule out other health problems, your doctor may order lab tests and imaging tests. You’ll also be asked to answer detailed questions about your health, feelings, thoughts, and daily habits. How you respond will help your doctor decide if you are in a schizophrenia prodrome and if so, what kind.
To reach the right diagnosis, your family doctor may refer you to a psychiatrist who treats schizophrenia.
Here Are Some Things You Can Do To Help Your Loved One:
- Help them get treatment and encourage them to stay in treatment
- Remember that their beliefs or hallucinations seem very real to them
- Tell them that you acknowledge that everyone has the right to see things their way
- Be respectful, supportive, and kind without tolerating dangerous or inappropriate behavior
- Check to see if there are any support groups in your area
Some symptoms require immediate emergency care. If your loved one is thinking about harming themselves or others or attempting suicide, seek help right away:
- Call the National Suicide Prevention Lifeline at 1-800-273-TALK or text the Crisis Text Line .
Read Also: What Is Feretrophobia
Seven Classes And The Key Findings That Shaped Them
The seven phenoclasses, as the U-M team has dubbed them, include standard measures doctors already use to diagnose and track the progress of bipolar disorder.
-
Changes in cognition, which includes thinking, reasoning and emotion processing
-
Psychological dimensions such as personality and temperament
-
Measures of behaviors related to substance use or abuse called motivated behaviors
-
Aspects of the persons life involving family, intimate relationships and traumas
-
Patterns of sleep and circadian rhythms
-
Measures of how patients symptoms change over time and respond to treatment
Some of the key findings the U-M team made in the Prechter cohort include:
Although bipolar disorder tends to run in families, the long-term study revealed no one gene explains it, says McInnis, who is the Woodworth Professor of Bipolar Disorder and Depression in the U-M Medical Schools Department of Psychiatry.
If there was a gene with a strong effect like what we see in breast cancer, for instance, we would have found it, he explains. We hope this new framework will provide a new approach to understand this disorder, and other complex diseases, by developing models that can guide a management strategy for clinicians and patients and give researchers consistent variables to measure and assess.
A Higher Risk Of Depression
In females, research suggests that bipolar II is more common than bipolar I. A person with bipolar II experiences depression and hypomania, a less extreme form of mania.
In females with bipolar disorder generally, depressive symptoms are more likely to be dominant. In fact, females with the condition are twice as likely to experience depression as males. Females are also more likely to experience psychosis with depression.
Because depressive symptoms tend to be dominant, females with bipolar disorder often receive an incorrect diagnosis of depression.
Recommended Reading: What Is The Meaning Of Phobia
Recommended Reading: What Is The Phobia Of Long Words
Know The Signs And Symptoms Of Bipolar
These symptoms may come before or after a hypomanic episode in bipolar II disorder.
A bipolar disorder diagnosis may be delayed because those closest to the individual didnt realize the behavior indicated a bigger issue or the first diagnosis of another condition was inaccurate. Pregnancy and seasonal affective disorder might be considered as causes for symptoms.
A mental health professional will determine if a manic or depressed episode has previously been experienced, and will also ask about the individuals behaviors and experiences over a course of time. A mood-disorder questionnaire with 13 questions is often used as an important diagnostic tool to assess symptom clusters and to avoid misdiagnosis.
In a survey by the National Depressive and Manic-Depressive Association , 69% of patients with bipolar disorder are misdiagnosed initially and more than one-third remained misdiagnosed for 10 years or more.
As you learn more about the whys, whos, and whats, its important to remember that although bipolar disorder is a lifelong condition, you can manage your mood swings and other symptoms by following a treatment plan. In most cases, bipolar disorder is treated with medications and psychological counseling .
Recommended Reading: Phobia Def
Cognitive Symptoms & Thinking Problems
These symptoms reflect how well the personâs brain learns, stores, and uses information.
Someone with schizophrenia might have a hard time with their working memory. For example, they may not be able to keep track of different kinds of facts at the same time, like a phone number plus instructions.
Along with having trouble paying attention, it can be hard for them to organize their thoughts and make decisions.
Show Sources
Recommended Reading: Prodromal Symptoms Of Schizophrenia Are Evident
What Does Schizophrenia Look Like When It Gets Better
As the symptoms of schizophrenia get better, people with this illness often become more involved socially. They may start dating again or they may spend more time with family and friends. The return to school or work, if this is possible for their circumstances, can provide structure that helps them remain stable.
Other Family Environmental Factors

In the British 1946 Birth Cohort, schizophrenia in offspring has been linked with problems in mothers general understanding and management of their children . Goldstein concluded that communication deviance in the family increased the risk for schizophrenia. Having a positive relationship with both the mother and father might be protective against schizophrenia among high-risk children. These findings may be explained by geneenvironment interaction.
In Finnish studies some possible stress factors have not generally been linked to schizophrenia. Very early temporal separation from parents and transfer to adequate nursing homes immediately after birth because of tuberculosis in the family did not predict schizophrenia, and neither did living in a single-parent family in childhood, low socio-economic status, or the size of the family of origin and multiparity. The connection between childhood socio-economic status and schizophrenia is not yet entirely resolved. Low or high socio-economic status in the family of origin has been found to be at least a modest risk factor for schizophrenia in some studies, while other studies report no increased risk.
Recommended Reading: What Assessment Findings Mark The Prodromal Stage Of Schizophrenia